Texas A&M Researchers Study Brain Cancer To Improve Treatments For People, Dogs
Story by Melissa Espinoza, Texas A&M College of Veterinary Medicine & Biomedical Sciences

Dr. Beth Boudreau, an assistant professor of neurology, welcomes Patches’ family to the Texas A&M College of Veterinary Medicine & Biomedical Sciences’ (CVMBS) Small Animal Hospital (SAH).
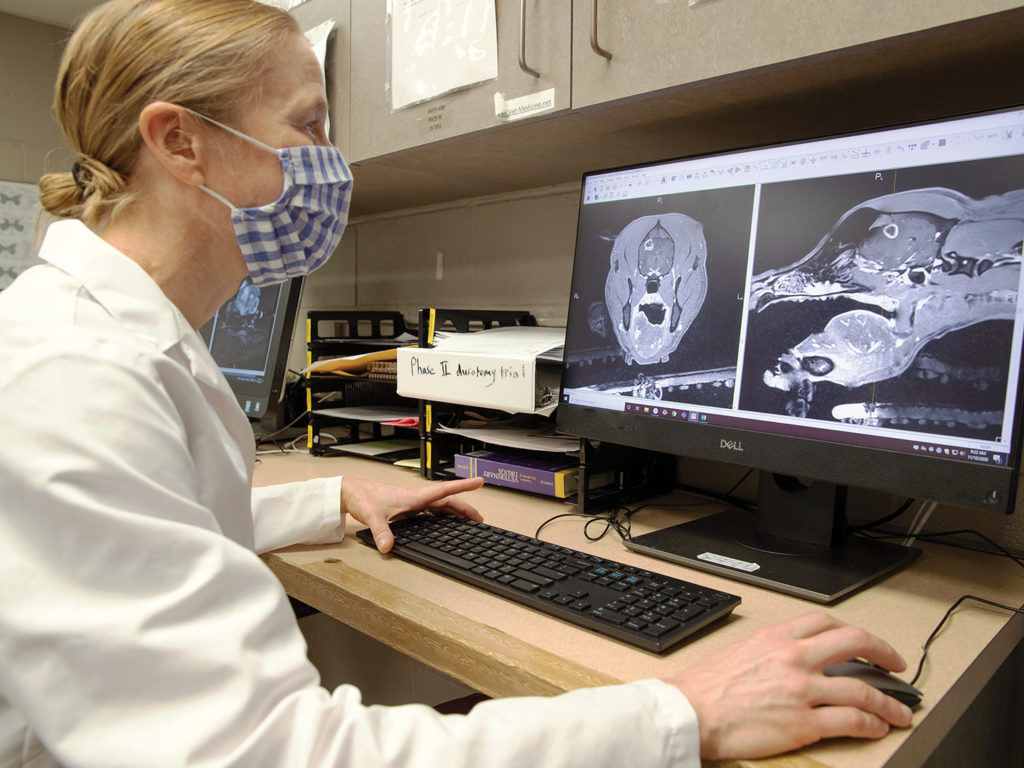
Patches, a sweet and playful dog, is visiting the SAH to be treated for a glioma, a form of cancer that grows in the brain and spinal cord. She is prepped, put under anesthesia, and sent for an MRI brain scan.
The veterinary team patiently waits for the images to load and for measurements to be taken, but the wait was worth it—Patches’ brain tumor appears smaller!
Not only is this good news for Patches and her family, but it’s also good news on a larger scale for Boudreau and her research team, who have been working for years to understand the tricky tumors.
Boudreau and her team of CVMBS researchers are collaborating with the Jackson Laboratory for Genomic Medicine and The University of Texas MD Anderson Cancer Center to test a new immunotherapy drug through a clinical trial.
This is important work because gliomas also occur in people and are the second-most common type of brain cancer in dogs.
Unfortunately, this type of cancer tends to have a poor prognosis—gliomas are difficult to surgically remove and traditional therapy comes with multiple side effects and a big bill. Even after a high-risk surgery to remove the tumor, plus weeks of radiation therapy and/or chemotherapy, dogs may only survive a few more months.
But Boudreau and her colleagues want to do better.
Time Is Precious
In addition to personal experiences with intracranial cancer, the research team is especially committed to finding a treatment for gliomas because of their distinctly poor prognoses.
“There are a lot of things about it—besides the short survival time and the fact that it tends to affect many younger individuals—that make it especially difficult,” Boudreau said. “Anyone who’s had a family member or a pet with a brain tumor has dealt with these same things to some degree—the fear, the uncertainty, the really wanting to try to do anything to get more good time.
“It might be that a quarter of their survival time is taken up with dealing with this very difficult treatment,” Boudreau said. “We don’t just want to extend the number of days; we want to extend the number of days that they get to spend together, having fun.”
Know Thy Enemy
This project started about five years ago when Dr. Jon Levine, a neurology professor and head of the CVMBS Small Animal Clinical Sciences department, made contact with MD Anderson.
“They were originally curious about this idea that dogs happen to share that tumor type with humans,” Boudreau said. “We still don’t know why these tumors arise.”
In people, researchers analyze environmental exposures, diet factors, and immune stimulations that “might predispose or protect” certain people with respect to this type of tumor.
“Dogs share our lives so intimately that if these factors are important for people, it’s not so surprising that our pets that share our lives would also get them,” Boudreau said.
To learn how these tumors work and how they relate to similar human tumors, researchers analyzed a massive canine genomic dataset collected from multiple glioma samples. They found that the tumors are, indeed, molecularly similar, suggesting that the two diseases have a similar mutational, cancer-causing process.
This means that treatments could be similar, as well.
Now, the team has developed a brand-new immunotherapy drug and are conducting clinical trials with dogs at the SAH.
A Targeted Therapy
“We don’t just want to extend the number of days; we want to extend the number of days that they get to spend together, having fun.“
DR. BETH BOUDREAU
When a dog is diagnosed with a glioma, Boudreau will meet with pet owners to discuss treatment options and her clinical trial. If the family agrees to try the experimental drug, the procedure is scheduled.
The dog gets MRI images taken that will guide the surgeons in administering the therapy before the patient is taken to an operating room, where the Brainsight system is set up to point a needle directly at the glial tumor. A small hole is drilled into the skull so the needle can pass and then the experimental drug is injected directly into the tumor.
If recovery goes well, the dog can go home the next day. In about a month, the dog comes for a repeat MRI to assess if the tumor has decreased in size.
“With this therapy, we’re trying to make tumors that do not, on their own, generate a lot of immune response and turn them into tumors that do by injecting them with this immunotherapy agent,” Boudreau said. “We also have the option to repeat the injection, because, as you know, with getting a vaccine, when you’re trying to stimulate the immune system, sometimes you get a better response if you do it more than once.”
These clinical trials are only the beginning.
“It’s really similar to what’s going on with the (COVID-19) vaccine development everyone is talking a lot about,” Boudreau said. “We need to establish that the drug is safe, and we need to establish that it is efficacious.”
After Boudreau’s data are published, her collaborators at MD Anderson can apply to test the therapy in a human clinical trial to attempt to establish the same results.
“Eventually, hopefully, we will be able to make it an approved treatment for people as well,” Boudreau said. “But it’s a long road.”
Breed Bias
While the team’s main focus is the clinical trial, Boudreau said the genetic analysis is an important piece of the project.
“Some breeds of dogs get gliomas a lot more than others. Boxers and Boston terriers are two big ones and then pit bulls,” she said. “What we’re trying to look at now is differences in the tumors from those breeds of dog, compared to the tumors from breeds of dog that just tend to get them sporadically.”
So far, six patients have had the experimental injection and two are still enrolled. The team hopes to have answers by the time they reach 21 trials.
Teamwork Makes The Dream Work

To get to this point, the Jackson Laboratory helped analyze the genes and cell regulation of the tumors, and using this information, scientists at MD Anderson, like biochemist Dr. Mike Curran, created the test drug. The CVMBS is now doing clinical trials on the drug. If this works, researchers like MD Anderson’s Dr. Amy Heimberger can help make the drug ready for people.
“The benefit of collaboration is huge because none of us could do this alone,” Boudreau said. “My goal and Dr. Heimberger’s goals are actually probably different. I want a way to treat this tumor in dogs, and, of course, I’m sure she’d be happy about that because she loves dogs, but her patients are people. So, it’s great that we can work together.
“And then our genomic study has given us more confidence that these tumors are really very similar and will respond similarly,” she said. “But in the end, what I’m hoping for is that we have something better to offer the owners because right now, we’re so limited.”
While, so far, the outcomes have been promising, science takes time.
“I didn’t know how long these things could take and how many things can get in your way; there are so many variables,” she said. “It’s really a good thing that we have a lot of people working on this from different angles, because, otherwise, we would never be able to explore enough possibilities fast enough.”
Grateful Looking Back, Hopeful Looking Forward
“We could not do this without our patients—our trial enrollees—and their families,” Boudreau said. “I’m always surprised when they express gratitude to us, because I feel so grateful for them. When they say that in the midst of all of these other things that they’re dealing with on a personal level that they want to help other dogs, too, and they want to help fight this disease, I feel like I’m meeting my people.”
Because they still need at least 14 dogs to complete their trial, Boudreau said recruitment is key in this project.
“If you have a dog or know someone who has a dog, especially if it’s a Boston terrier or a Boxer who has signs of something going on in his or her brain, we’d like you to come see us,” she said. “Even if it’s not a glioma, there might be something we can help with.
“If it does happen to be a glioma, we would love to try to help out any way we can,” she said. “We have this trial, which is not widely available, and we hope that that’s going to be an avenue to help some pets that wouldn’t otherwise be able to get help.”
Boudreau is hopeful and optimistic, much like the families that enroll their dogs in her study.
“When owners enroll, what they’re looking for is something they can do, because it gives them a source of hope. When they can’t do any of the other treatments but find out they can try this for their pet, I have to explain to them that it might not actually be effective; there could be complications,” she said.
“But at the end of the day, the ones who sign up say they’re just happy to have something they can try that gives them hope for the next day. When we send the patients home after their injection, because they’re doing well enough to go home and we walk down that hallway to the front door, that makes it worth it. Every time.”
###
Note: This story originally appeared in the Spring 2021 edition of CVMBS Today.
For more information about the Texas A&M College of Veterinary Medicine & Biomedical Sciences, please visit our website at vetmed.tamu.edu or join us on Facebook, Instagram, and Twitter.
Contact Information: Jennifer Gauntt, Director of CVMBS Communications, Texas A&M College of Veterinary Medicine & Biomedical Sciences; jgauntt@cvm.tamu.edu; 979-862-4216


